Preliminary results from the International Infant Hydrocephalus Study
By: Maggie A. Khuu and Dr. Jenna Koschnitzky, Director of Research Programs
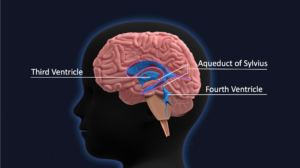 Aqueductal stenosis, a narrowing of the cerebral aqueduct that blocks the flow of cerebrospinal fluid (CSF) between the third and fourth ventricles, can lead to the development of hydrocephalus. In infants that suffer from this condition, two common treatment options are available: implantation of a shunt or an endoscopic third ventriculostomy (ETV). In the ETV procedure, an endoscope is used to puncture the membrane in the floor of the third ventricle and create a pathway to allow CSF to flow out into the ventricular space.
Aqueductal stenosis, a narrowing of the cerebral aqueduct that blocks the flow of cerebrospinal fluid (CSF) between the third and fourth ventricles, can lead to the development of hydrocephalus. In infants that suffer from this condition, two common treatment options are available: implantation of a shunt or an endoscopic third ventriculostomy (ETV). In the ETV procedure, an endoscope is used to puncture the membrane in the floor of the third ventricle and create a pathway to allow CSF to flow out into the ventricular space.
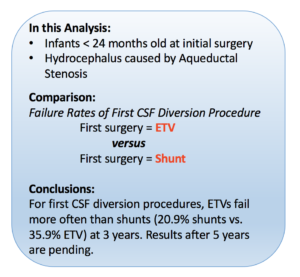
The International Infant Hydrocephalus Study (IIHS), composed of more than twenty different medical centers from around the world, pooled together data to better understand how aqueductal stenosis patients (<24 months old) fared with ETV treatment compared to shunt treatment. They wanted to know whether patient outcomes at five years of age were more successful with initial ETV treatment over initial shunt treatment. While the five year outcome results are still pending, preliminary results at 3 years revealed that patients that received initial shunt implantation had lower risk for failure compared to patients that received initial ETVs (20.9% shunts vs. 35.9% ETV). Failure was defined as need for need for repeat CSF diversion procedures (either ETV or shunt) or death due to hydrocephalus. ETV failure can be attributed to the closure of the hole in the floor of the third ventricle or a subsequent blockage by other cells/tissue.
However, does ETV failure affect subsequent treatment outcomes? After ETV failure, patients have the option to undergo a repeat ETV or undergo shunt implantation. Researchers from the IIHS sought to determine whether or not previous ETV treatment had a positive effect on shunt implantation. It has been hypothesized that previous ETV can have a protective effect on shunt insertion with some researchers advocating for simultaneous ETV and shunt treatments.
At this time, the IIHS reported was that there was no significant difference in failure outcomes with shunts implanted after a failed ETV compared to shunts placed as the initial CSF diversion procedure. Their findings indicate that initial ETV treatment neither benefits nor worsens subsequent shunt implantation.

However, it is important to note that these results were limited to a very small sampling of patients and only in infants with aqueductal stenosis. It is not yet known whether these results are applicable to broader populations of hydrocephalus patients. These limitations call for a larger study to be established to better determine how widely their findings may apply.
