Hydrocephalus in Pregnancy
Why do Babies Develop Hydrocephalus?
Hydrocephalus that is present at birth is referred to as congenital hydrocephalus. Congenital hydrocephalus is caused by a complex interaction of genetic and environmental factors during fetal development. The most common causes of congenital hydrocephalus are:
- Aqueductal stenosis
- Brain malformations (for example Dandy-Walker Syndrome and Chiari Malformation)
- Spina bifida
How is Hydrocephalus Diagnosed in Pregnancy?
Hydrocephalus can be detected using a normal ultrasound examination, which is typically performed throughout a woman’s pregnancy.
During ultrasound screening, the technician may see pockets of fluid in the developing brain, indicating enlarged ventricles and the possible presence of hydrocephalus.
Hydrocephalus can be detected as early as the latter part of the first trimester. Diagnosis has been made as early as 13 weeks. Around 20 to 24 weeks, abnormal dilation of the ventricles are more clearly detectable.
In certain special cases, fetal magnetic resonance imaging (MRI) may be done, especially when abnormal anatomy is observed with ultrasonography. The MRI provides more detailed images of the brain.
For more detailed information on Hydrocephalus, visit About Hydrocephalus.
Monitoring Hydrocephalus in Pregnancy
Hydrocephalus during pregnancy is managed by observing your baby (fetus) with regular ultrasounds. At this time, there is no fetal treatment for this condition.
Throughout the pregnancy, it is important to have a series of ultrasounds to monitor ventricular size. There is no way to predict whether the ventricular size will increase or decrease in subsequent studies.
It is generally felt that if ventricular size remains stable the fetus should be followed to term.
The best way to improve the outcome for the baby is to delay delivery until the fetus is as mature as possible. Your doctors will also determine if a vaginal delivery is an option, or if a cesarean birth is recommended due to the size of your baby’s head.
If progressive ventriculomegaly (that is if the ventricles continue to enlarge) is demonstrated several options are considered:
- For fetuses younger than 32 weeks, the risk of pulmonary (lung) immaturity must be weighed against the potential damage of progressive ventriculomegaly and early delivery.
- For fetuses with a diagnosis of spina bifida, pre- or post-natal surgery is an option to close the baby’s back before or right after birth. To learn more about pregnancy and spina bifida, visit the Spina Bifida Association’s Expectant Parents Guide.
- For fetuses older than 35 weeks, a preterm cesarean section may be performed, and a shunt may be placed postnatally (after birth).
Once hydrocephalus in pregnancy is suspected, establishing a relationship with a pediatric neurosurgeon as early as possible is critical. Your baby may need to undergo treatment quickly after birth. The pediatric neurosurgeon can provide you with details and the best treatment option for your child.
To find a pediatric neurosurgeon and/or neurologist, visit our Physicians’ Directory.
How is Hydrocephalus Treated in Babies?
The goal of treatment is to reduce the pressure inside your child’s brain by draining the excess fluid, cerebrospinal fluid (CSF).
A detailed neurological exam at birth, along with an examination of the head size and soft spots (fontanels) will be done to verify the diagnosis of hydrocephalus.
If there is increased pressure on the brain at birth, hydrocephalus is treated with one of three surgical options:
Shunt System
The most common treatment for hydrocephalus is a medical device called a shunt.
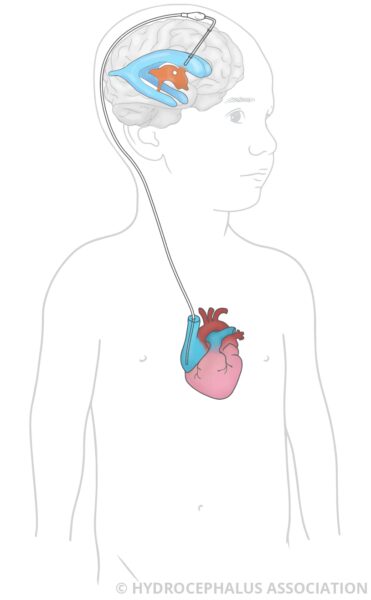
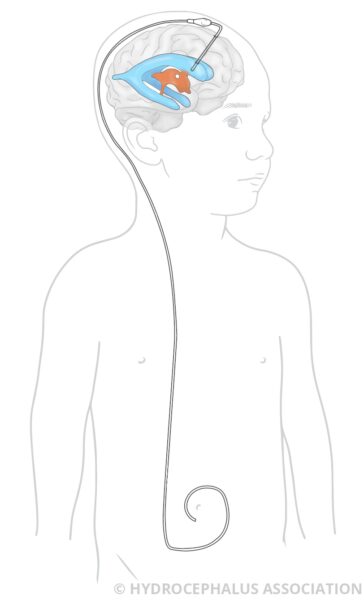 A shunt is a device that allows the pressure in the brain to normalize by draining the fluid to another part of your child’s body, most often the abdominal cavity, where the fluid can be reabsorbed. The tube from the brain is connected to a valve that helps to regulate how much fluid leaves the brain.
A shunt is a device that allows the pressure in the brain to normalize by draining the fluid to another part of your child’s body, most often the abdominal cavity, where the fluid can be reabsorbed. The tube from the brain is connected to a valve that helps to regulate how much fluid leaves the brain.
The goal of placing this shunt is to allow for normal brain development.
To learn more about a shunt, visit Shunt Systems and What to Expect with Hydrocephalus Shunt Surgery.
Endoscopic Third Ventriculostomy (ETV)
The ETV surgical treatment option is typically used for children over the age of 2 with non-communicating (obstructive) hydrocephalus; hydrocephalus caused by a blockage in the brain like aqueductal stenosis. Not everyone is a candidate for ETV treatment.
Endoscopic Third Ventriculostomy (ETV) with Choroid Plexus Cauterization (CPC)
The third treatment option involves an ETV with the addition of a procedure called choroid plexus cauterization (CPC). This treatment is primarily used in children under 2.
To learn more about ETV and ETV/CPC, visit ETV and ETV with CPC and What to Expect with ETV Surgery.
What is the Prognosis for Babies with Hydrocephalus?
Many babies born with hydrocephalus go on to lead full lives, though the road you envisioned for your child might not be the road you journey down together.
Do not despair! Babies with hydrocephalus grow into resilient and determined children.
Know That You’re Not Alone.
Pregnancy is a joyous time for a woman. However, receiving the news that your developing baby has hydrocephalus can be overwhelming, frightening, and sad for expectant women and couples.
We provide programs and support services to help you navigate your child’s journey with hydrocephalus. Our organization will help you connect with other parents, trained volunteers, and medical professionals to help build a strong support system.
For support and resources, visit Help and Support.
Research and Hydrocephalus
As the leading private funder of hydrocephalus research in the country, we are investing in research to improve outcomes as well as prevent the development of hydrocephalus and, ultimately, find a cure. The Hydrocephalus Clinical Research Network (HCRN) is a network of children’s hospitals that conduct clinical research to improve treatment and care for babies and children with hydrocephalus.
You can be a part of the research. Enroll in HAPPIER, the only hydrocephalus patient-powered registry in the country, and help our doctors and scientists better serve you!
Join the HA Patient Powered Interactive Engagement Registry to accelerate hydrocephalus research.
Information you can trust! This article was produced by the Hydrocephalus Association, copyright 2023. We would like to thank the following individuals for their valuable contributions and expert input: Marion L. (Jack) Walker, MD, and Cathy Cartwright, DNP, RN-BC, PCNS, FAAN.
