Hydrocephalus in Infants and Children
In simplest terms, hydrocephalus is extra fluid in the brain.
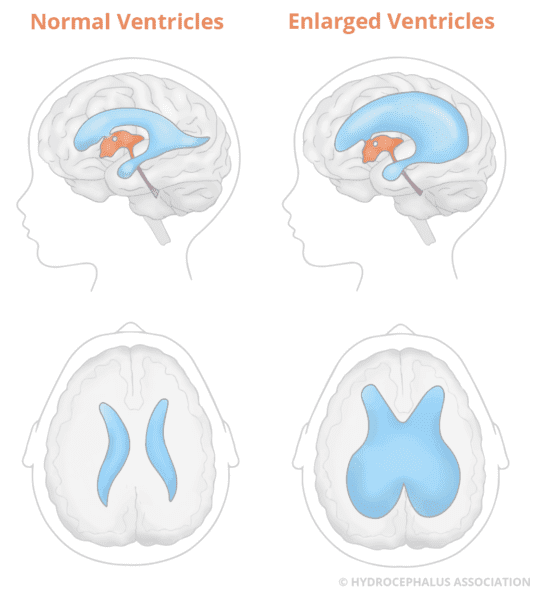
The fluid, cerebrospinal fluid (CSF), is found within spaces (cavities) in the brain which are called ventricles. The main purpose of CSF is to cushion and protect the brain and the spinal cord.
The goal of treatment is to relieve the pressure inside your child’s head by regulating the amount of fluid within the ventricles.
What Causes Hydrocephalus in Infants and Children?
Hydrocephalus can develop for a variety of reasons.
 Hydrocephalus that is present at birth is congenital hydrocephalus.
Hydrocephalus that is present at birth is congenital hydrocephalus.
Congenital hydrocephalus is caused by a complex interaction of genetic and environmental factors during fetal development.
The most common causes of congenital hydrocephalus are:
- Aqueductal Stenosis
- Brain malformations (for example Dandy-Walker Syndrome and Chiari Malformation)
- Spina bifida
Hydrocephalus that develops later in life in some children, teens, and even in adults, but is caused by a condition that existed at birth, is still considered a form of congenital hydrocephalus.
Hydrocephalus that develops after birth is acquired hydrocephalus.
The most common causes are:
- Head injuries
- Brain tumors
- Intraventricular hemorrhage (brain bleed)
- Meningitis or other infection of the brain or spinal cord
Both children, teens, and adults can be diagnosed with acquired hydrocephalus.
There are other classifications that you might hear when talking to your doctor, particularly around the time of diagnosis. These can include:
- Compensated or arrested hydrocephalus
- Communicating hydrocephalus
- Non-communicating hydrocephalus, also known as obstructive hydrocephalus
For more detailed information on the types and causes of hydrocephalus visit this page.
What are the Symptoms of Hydrocephalus in Infants and Children?
The signs and symptoms can appear differently for each child, especially depending on your child’s age and how far along the condition is at the time of diagnosis.
Symptoms in Infants and Toddlers
In an infant, the most obvious sign is an unusual enlargement of the baby’s head as it expands in response to the outward pressure created by the extra fluid. This is because the bones of the skull are not yet closed, therefore allowing the head to expand. As an infant grows, the bones will naturally meet and fuse. You might hear your medical team refer to these as the suture lines.
NOTE: Young toddlers whose sutures have not yet closed may also show signs of head enlargement.
Additional signs may include:
- The soft spot, or fontanel, on the top of the head, may be tense and bulging
- The scalp may appear thin and glistening
- The scalp veins may appear to have unnatural fullness (prominence)
Physical symptoms to watch for may include:
- Vomiting
- Excessive tiredness
- Fussiness
- Poor feeding
- Downward deviation of the baby’s eyes (the sun-setting sign where your baby’s eyes are stuck looking down)
- Seizures
Symptoms in Children and Adolescent
Once an infant’s sutures have closed, the fluid has nowhere to go and builds up, causing pressure on the brain, a term that is referred to as raised intracranial pressure (ICP).
Physical symptoms may include:
- Headaches
- Nausea and/or vomiting
- Vision problems (blurred or double vision)
- Fatigue and/or sleepiness (older children may have difficulty waking up and staying awake)
- Poor appetite
- Problems with balance
Cognitive or behavioral changes may include:
- Changes in personality and/or more irritability than normal
- Inability to concentrate
- Hard time remembering things
- School performance may decline
- Delayed development (or problems with previously acquired skills) in such areas as walking or talking, or poor coordination
While at times the symptoms are very noticeable, other times they can be very subtle and progress so slowly that only in retrospect are they appreciated.
How is Hydrocephalus Diagnosed in Infants and Children?
There are numerous tests that can help diagnose hydrocephalus.
The first and simplest test is measuring a baby’s head circumference at birth and during routine visits with your pediatrician. If your baby’s head is larger than normal or if there is a rapid increase in the head size, your doctor will refer you to a specialist (neurosurgeon).
For toddlers and older children, it may be a neurological evaluation that warrants a referral to a specialist and further diagnostic testing, which typically includes brain imaging techniques such as ultrasonography (US), computed tomography (CT), and magnetic resonance imaging (MRI).
Brain Imaging Techniques
Ultrasound is used in infants with open soft spots or fontanels. The ultrasound has no ill effects on the brain, it is painless, and it requires no sedation. It provides adequate visualization of the lateral ventricles, but other parts of the brain are not so well seen.
CT scan is a reliable procedure for diagnosing and assisting in the management of hydrocephalus. A CT Scan is a sophisticated technique in which X-ray beams are passed through a patient’s body and pictures of the internal structures, in this case, the brain, are made by the computer. CT scans can usually be performed without sedation.
Note: CT scans use higher doses of radiation compared to simpler imaging tests. Improvements in CT equipment, however, have allowed for better images at lower doses for children. These are referred to as low-dose CT scans.
 MRI (Magnetic Resonance Imaging) uses radio signals, a large magnet, and a computer to scan your child’s body. The signals are then developed into images by the computer.
MRI (Magnetic Resonance Imaging) uses radio signals, a large magnet, and a computer to scan your child’s body. The signals are then developed into images by the computer.
NOTE: Like the CT scan, it is a diagnostic technique that produces images of the brain-but unlike CT scanning, MRI does not use x-rays/radiation. Instead, MRI uses radio signals and a very powerful magnet to scan your child’s body, and the signals are then formed into pictures by a computer. MRI is a painless procedure and has no known side effects.
There are two types of MRI scans:
The Single Shot Fast Spin Echo (also called a ‘quick brain MRI), which takes about three minutes and rarely requires sedation, is used to assess ventricular size.
The full MRI, which takes 30 to 60 minutes and may require sedation, shows more minute details. Before the longer scans are performed, your child may be given a sedative to minimize movement that would cause blurring of the images.
At this point in the diagnostic process, it is important that a neurosurgeon become part of your medical team, along with your primary care physician. Their involvement from the diagnostic stage onward is helpful not only in interpreting test results but also in selecting candidates for shunt surgery.
They should also discuss the actual surgery and follow-up care, as well as outcomes and possible complications of surgery.
To find a pediatric neurosurgeon and/or neurologist, visit our Physicians’ Directory.
How is Hydrocephalus Treated in Infants and Children?
While there is currently no known way to prevent or cure hydrocephalus, there are three life-saving treatment options that require brain surgery.
Shunt System
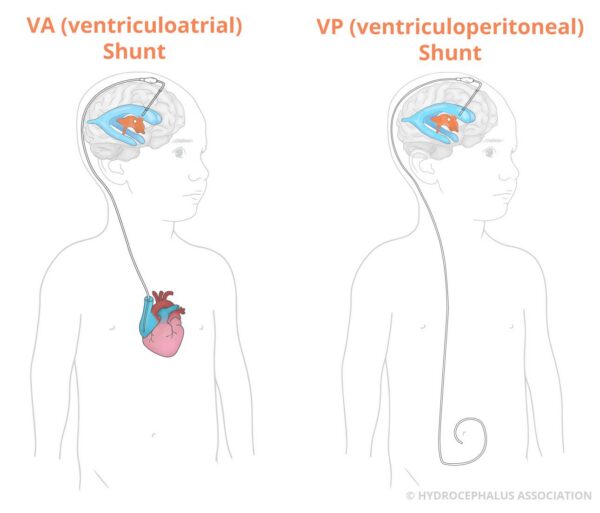 The most common treatment for hydrocephalus is a medical device called a shunt. The purpose of the shunt is to reduce the pressure inside your child’s brain by draining the excess fluid, cerebrospinal fluid (CSF). The shunt diverts the fluid to another part of your child’s body, most often the abdominal cavity or heart where it can be absorbed.
The most common treatment for hydrocephalus is a medical device called a shunt. The purpose of the shunt is to reduce the pressure inside your child’s brain by draining the excess fluid, cerebrospinal fluid (CSF). The shunt diverts the fluid to another part of your child’s body, most often the abdominal cavity or heart where it can be absorbed.
To learn more about a shunt, please visit our Shunt System page and What to Expect with Hydrocephalus Shunt Surgery page.
ETV (Endoscopic Third Ventriculostomy)
A second surgical treatment option, ETV, is typically used for children over the age of 2 with non-communicating (obstructive) hydrocephalus; hydrocephalus caused by a blockage in the brain like aqueductal stenosis. The endoscope creates an alternative pathway for CSF to flow out of the ventricles and around the brain. A shunt is not needed. Not everyone is a candidate for ETV treatment.
CPC (ETV with Choroid Plexus Cauterization)
The third treatment option involves an ETV with the addition of a technique that burns or cauterizes the choroid plexus tissue to reduce the amount of fluid being introduced into the ventricles. This is referred to as choroid plexus cauterization or CPC. This treatment is primarily used in children under 2. Not everyone is a candidate for ETV/CPC treatment. ETV/CPC is a very technical surgery and should be performed by a neurosurgeon trained and experienced in the procedure.
To learn more about ETV and ETV/CPC, please visit our ETV and ETV with CPC page and What to Expect with ETV Surgery page.
What are Possible Complications After Surgery for a Child with Hydrocephalus?
It is important to understand that life with a shunt or ETV requires you to always be well-informed and vigilant about complications. While some people can go 20 years or more without a complication, with a complex condition like hydrocephalus, things can change quickly, therefore it’s critical to be prepared.
Complications of a Shunt
Sometimes shunts can malfunction (fail) or become infected. Some of the signs and symptoms to watch for include:
- Enlargement of baby’s head
- Fontanel is full and tense when an infant is upright and quiet
- Headache
- Vomiting
- Visual changes
- Irritability or fussiness
- Sleepiness
- Difficulty waking up or staying awake (this symptom requires urgent attention as it can potentially lead to a coma)
- Redness along the shunt tract, potentially present with shunt failure or infection
Your child may require a shunt revision, which requires another brain surgery. Please contact your child’s healthcare provider right away.
Complications of an ETV
An ETV can close at any time and put an individual in an emergency situation. It is critical to understand the signs and symptoms of closure of an ETV. The symptoms are often similar to those of shunt failure. When an ETV fails it requires another brain surgery to reopen the hole.
See our page on ETV complications for a detailed list of signs and symptoms.
What is the Prognosis for Infants and Children with Hydrocephalus?
Many children with hydrocephalus go on to lead full lives, though the road you envisioned for your child might not be the road you journey down together.
What can you expect?
Each child is different and hydrocephalus can present varying degrees of cognitive and physical challenges based on the cause of the hydrocephalus and the clinical course.
Shunt Revisions
It is not uncommon for babies who have shunts to need repeated shunt revisions in the first weeks, months, or years as their bodies adjust to the condition and treatment. Repeated brain surgeries can impact a baby’s normal development for many reasons including repeated intervention in the brain and time away from being able to grow and learn.
Additional Medical Conditions
In addition to hydrocephalus, some children may be diagnosed with other medical conditions, including but not limited to seizures, cortical visual impairment, cerebral palsy, spina bifida, Dandy-Walker Syndrome, and Chiari Malformation, among others.
Development Challenges
Some of the challenges we see in babies as they grow include:
- Delays in meeting milestones
- Sensory issues
- Problems with chewing and/or swallowing
- Eye-hand coordination
- Visual-spatial deficits
- Delayed speech
- Delayed gross motor development like rolling over, crawling, and walking
Do not despair! Babies with hydrocephalus grow into resilient and determined children.
With advances in medical treatments, therapies, educational support services, and an entire industry around toys and games to stimulate the brain and encourage learning, most children grow up to fulfill their dreams of making friends, playing sports, winning academic awards, graduating from high school, and going to college.
To learn more about physical activities view our page “Staying Active”.
“The two things that made the difference in our lives were to learn as much as I could about the condition and get involved with HA and meet other parents. Even though my family loves me, they don’t quite understand what we’re going through, but the other parents raising children with hydrocephalus do.” – Denise
Information you can trust! This article was produced by the Hydrocephalus Association, copyright 2023. We would like to thank the following individuals for their valuable contributions and expert input: Marion L. (Jack) Walker, MD, and Cathy Cartwright, DNP, RN-BC, PCNS, FAAN.

 Hydrocephalus that is present at birth is congenital hydrocephalus.
Hydrocephalus that is present at birth is congenital hydrocephalus.