About Hydrocephalus
What is Hydrocephalus?
Hydrocephalus is a chronic, neurological condition caused by an abnormal accumulation of cerebrospinal fluid (CSF) within the cavities (ventricles) of the brain.
Hydrocephalus happens when there is an imbalance between the amount of CSF produced and the rate at which it is absorbed. As the CSF builds up, it causes the ventricles to enlarge, putting increased pressure on the brain.
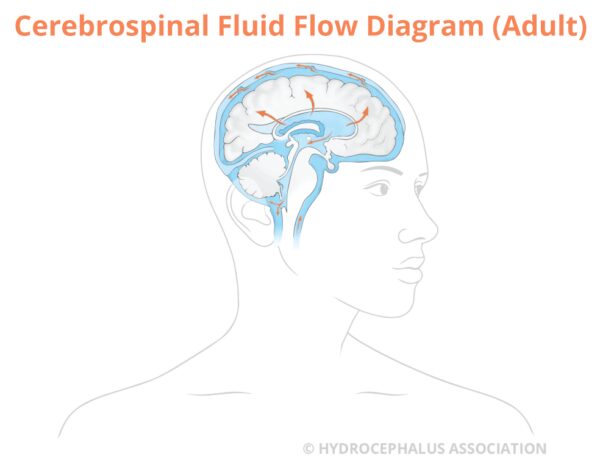
The brain produces a clear fluid called, cerebrospinal fluid (CSF), that surrounds and protects the brain and spinal cord. CSF is mostly produced in the ventricles and the choroid plexus. It circulates through the ventricular system in the brain and is absorbed into the bloodstream. CSF is in constant circulation and has many functions. It surrounds the brain and spinal cord and acts as a protective cushion against injury. CSF contains nutrients and proteins that are needed for the nourishment and normal function of the brain. It carries waste products away from surrounding tissues. For more detailed information, visit How Cerebrospinal Fluid Works in Hydrocephalus.
Who Develops Hydrocephalus?
Hydrocephalus affects a wide range of people, from infants and older children to young, middle-aged and older adults.
- Over 1,000,000 people in the United States currently live with hydrocephalus.
- In the United States, 1 out of 770 babies develops hydrocephalus each year.
- NPH is most commonly seen in adults aged 60 or over. A recent study estimates that 800,000 older Americans may be living with NPH. This disorder often goes undiagnosed. It is estimated that more than 80% of cases remain unrecognized or untreated.
While there is currently no known way to prevent or cure hydrocephalus, it can be treated with surgical intervention.
Types and Causes of Hydrocephalus
Hydrocephalus can develop for a variety of reasons.
You can be Born with Hydrocephalus
Hydrocephalus present at birth, even if it surfaces later in life, is referred to as congenital hydrocephalus. It is caused by a complex interaction of genetic and environmental factors during fetal development.
The most common causes of congenital hydrocephalus are:
- Spina bifida
- Aqueductal stenosis
- Brain malformations (for example Dandy-Walker Syndrome and Chiari Malformation)
You can Acquire Hydrocephalus
Hydrocephalus that develops after birth is referred to as acquired hydrocephalus. Both children and adults can be diagnosed with it. The most common causes are:
- Head injuries
- Brain tumors
- Intraventricular hemorrhage (brain bleed)
- Meningitis (brain infection) or other infection of the brain or spinal cord
There are other classifications that you might hear when talking to your doctor, particularly around the time of diagnosis. These can include:
- Compensated or arrested hydrocephalus
- Communicating hydrocephalus
- Non-communicating hydrocephalus, also known as obstructive hydrocephalus
For more detailed information, visit Types and Causes.
You can Develop Hydrocephalus as an Older Adult
Hydrocephalus that occurs in older adults is referred to as normal pressure hydrocephalus (NPH) and is most commonly seen in adults aged 60 and older.
NPH differs from hydrocephalus in that the ventricles in the brain become enlarged, sometimes with little or no increase in intracranial pressure (ICP).
What are the Symptoms of Hydrocephalus?
The symptoms of untreated hydrocephalus vary, however, there are some overarching signs and symptoms of the condition.
Infants: Physical Symptoms
- Abnormal enlargement of the baby’s head
- A rapid increase in head circumference
- A bulging or tense fontanelle (soft spot on the baby’s head)
- Vomiting
- Excessive tiredness
- Downward deviation of the baby’s eyes, also called “sun-setting
To learn more and a detailed list of signs and symptoms, visit Hydrocephalus in Infants and Children.
Children: Physical and Cognitive Symptoms
- Headaches
- Nausea and/or vomiting
- Vision problems (blurred or double vision)
- Excessive tiredness (older children may have difficulty waking up and staying awake)
- Poor appetite
- Problems with balance
- Changes in personality and/or more irritability than normal
- Inability to concentrate
- Hard time remembering things
- Developmental delays or missed milestones
- School performance may decline
To learn more and a detailed list of signs and symptoms, visit Hydrocephalus in Infants and Children.
Young and Middle-aged Adults: Physical Symptoms
- Headaches
- Nausea or vomiting
- Vision problems (blurred or double vision)
- Excessive tiredness (Difficulty remaining awake or waking up)
- Difficulty with balance and coordination issues
- Disturbances in gait
- Vertigo
- Syncope (fainting)
- Memory problems, particularly short-term memory
To learn more and a detailed list of signs and symptoms, visit Hydrocephalus in Adults.
Older Adults with Normal Pressure Hydrocephalus (NPH): Physical Symptoms
Decreased normal functioning in three main areas:
- gait disturbances (difficulty walking or making turns, feeling like it’s hard to take the first step, balance issues, falling)
- cognitive impairment (feeling withdrawn, talking less, having a hard time paying attention, poor handwriting, trouble with simple math calculations),
- impairment in bladder control (trouble “holding it”, not being able to get to the bathroom fast enough, experiencing accidents)
Diagnosis of Hydrocephalus
Diagnosis During Pregnancy
During pregnancy, an ultrasound may detect enlarged ventricles, indicating the possible presence of hydrocephalus. In some cases, fetal magnetic resonance imaging (MRI) may be done, especially when abnormal anatomy is observed with ultrasonography. The MRI provides more detailed images of the brain and information about the extent and severity of hydrocephalus.
To learn more visit How is Hydrocephalus Diagnosed in Pregnancy?
Types of Tests for Infants, Children, and Adults
A diagnosis is made by using brain imaging techniques such as computed tomography (CT), magnetic resonance imaging (MRI), and a thorough neurological evaluation during a doctor visit.
To learn more visit Hydrocephalus in Infants and Children or Hydrocephalus in Adults.
Additional Types of Tests for Adults
More tests are often performed in adults in order to diagnose the condition. These tests may include lumbar puncture (spinal tap), continuous lumbar CSF drainage, intracranial pressure (ICP) monitoring, measurement of cerebrospinal fluid outflow resistance, or isotopic cisternography. A neuropsychological evaluation may also be recommended. The decision to order a particular test may depend on the specific clinical situation, as well as the preference and experience of the medical team.
Not all of the tests listed are required in order to make a diagnosis.
Is Hydrocephalus Treatable?
Yes, hydrocephalus is treatable with early detection and appropriate intervention. While brain surgery is currently the only form of treatment, many people find success in managing their hydrocephalus with one of the three following surgical options:
- Shunt: The most common treatment for hydrocephalus is a medical device called a shunt. This is a flexible tube that is placed in the ventricular system of the brain that diverts the flow of CSF to another part of the body, most often the abdominal cavity, or heart, where it can be absorbed. The shunt system has a valve that maintains CSF at normal pressure within the ventricles.
To learn more about shunt systems, visit Shunt Systems. - Endoscopic Third Ventriculostomy (ETV): With this procedure, an endoscope (a small tube with a camera) is used to puncture a hole in the membrane on the floor of the third ventricle. This opens a natural pathway that allows CSF to flow out of the ventricles and around the brain, bypassing a blockage. An ETV is an important alternative to shunting for some cases of obstructive hydrocephalus and may be useful in other cases as well. This treatment option is not suitable for everyone and it is typically used for patients over the age of 2 who have a non-communicating (obstructive) hydrocephalus, but can be considered in other situations, as well. Non-communicating hydrocephalus occurs when there is a blockage within the ventricles of the brain, like aqueductal stenosis.
To learn more about ETV, visit ETV and ETV with CPC - Endoscopic Third Ventriculostomy (ETV) with Choroid Plexus Cauterization (CPC): This surgery, primarily performed in infants, involves the addition of choroid plexus cauterization (CPC) to the ETV. The choroid plexus is a network of vessels in the ventricles of the brain where cerebrospinal fluid is produced. Once inside the brain, the neurosurgeon uses a device to burn, or cauterize, choroid plexus tissue to reduce the amount of fluid being introduced into the ventricles. The fluid then passes through the opening made during the ETV and into the space surrounding the surface of the brain. This treatment is primarily used in children under 2.
To learn more about ETV/CPC, visit ETV and ETV with CPC and What to Expect with ETV Surgery.
Note: Hydrocephalus during pregnancy is managed by observing your baby (fetus) with regular ultrasounds. At this time, there is no fetal treatment for this condition. Read more about monitoring hydrocephalus during pregnancy.

Understanding how a shunt works can be easier with a simple visual. My Hydro Bear has a shunt, offering a hands-on way to see what the device looks like, follow where the tubing goes, and explain the concept to children, teens, adults, or family members. Many people use it as an educational tool during conversations about surgery, appointments, and long-term care.
Hydrocephalus Treatment Complications
It is important to understand that living with a shunt or ETV requires being well-informed and vigilant about potential complications. While some people can go many years without experiencing any issues, hydrocephalus is a complex condition. Therefore, it’s critical to be prepared in case complications do arise.
Complications of a Shunt and an ETV
It is possible for a shunt to malfunction, fail, or become infected, which would then require a shunt revision (brain surgery). Likewise, an ETV can close unexpectedly and put an individual in an emergency situation. It is critical to understand the signs and symptoms of shunt failure or the closure of an ETV in order to respond quickly.
Seeking immediate medical attention can identify a resolvable complication and enable you or your family member to avoid brain damage or even death.
To learn more, explore our pages on Complications of Shunt Systems, ETV Complications, and Shunt Malfunction: Frequently Asked Questions.
What is the Prognosis?
Investments in research and advances in technology, as well as diagnostic and treatment protocols, are bringing hope to individuals with hydrocephalus, enabling them to lead full and active lives.
The long-term effects of hydrocephalus can vary greatly from person to person. While every individual’s experience is unique, there are some general problems we see across our patient population. These include, but are not limited to:
- learning challenges
- problems with vision
- short-term memory issues
- executive function challenges
- chronic headaches and pain
Navigating the journey with hydrocephalus can be filled with challenges and uncertainties, but we want you to know that you are not alone. We are here to provide you with essential tools and resources, empowering you to take control of your life. The Hydrocephalus Association fosters a supportive community across the country, ready to stand by you and your family every step of the way.
Information you can trust! This article was produced by the Hydrocephalus Association, copyright 2023. We would like to thank the following individuals for their valuable contributions and expert input: Marion L. (Jack) Walker, MD, and Cathy Cartwright, DNP, RN-BC, PCNS, FAAN.
