New views on Postinfectious Hydrocephalus
Dr. Jenna Koschnitzky, National Director of Research Programs
Many people are born with hydrocephalus, but hydrocephalus can also develop after injury, brain infection, or as part of the aging process. In a recent study published in Nature, Dr. Chay Kuo, out of Duke University, discovered a mechanism that may lead to the development of Postinfectious Hydrocephalus.
In the study, Dr. Kuo and his lab showed that some infections can make ependymal cells, the cells that line the ventricles, revert back into undifferentiated cells, meaning the final function of the cell has not been determined (these can be thought of as immature cells).
Why is this significant? As mentioned above, ependymal cells line the ventricles and separate the cerebrospinal fluid from the brain. The ependymal cells also have microscopic hair-like structures known as cilia.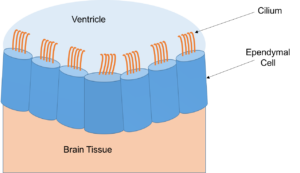
Other studies have shown that the movement of the cilia plays an important role in the movement of cerebrospinal fluid (CSF) and that hydrocephalus can develop if the cilia are damaged or missing.
When the ependymal cells revert back to undifferentiated cells, they lose their cilia. This could help explain why people with brain infections sometimes develop hydrocephalus.
In the paper, Dr. Kuo shows that the process of reverting from an ependymal cell to an undifferentiated cell occurs when a specific protein, Foxj1, stops being produced or is rapidly destroyed. Potentially, drugs that stabilize the protein may be used to stop the development of Postinfectious Hydrocephalus.
How common is Postinfectious Hydrocephalus? The risk of developing Postinfectious Hydrocephalus is dependent on the severity and type of infection. In developed countries, the rate of Postinfectious Hydrocephalus after neonatal meningitis is as high as 30%, and the rate of Postinfectious hydrocephalus after tubercular meningitis is a staggering 80-90%. In some developing countries, over 60% of hydrocephalus cases are postinfectious.
For more information on this study please visit: https://phys.org/news/2018-04-brain-cell-achilles-heel-prompt.html
To access the original journal article please visit: DOI: 10.1038/s41467-018-03812-w
