Living With NPH Part 1: Trying to Make Peace With a “New Normal”
Written By Frank Salamone, L.C.S.W. 
“I’m sailing a ship on stormy seas on the brightest of days.” – Michael J Fox.
I am living with normal pressure hydrocephalus (NPH). But I promise you; there is nothing normal about it.
NPH is often misdiagnosed as Alzheimer’s disease or Parkinson’s disease, stroke, or other neurodegenerative conditions. It can be difficult to diagnose because sometimes the symptoms are mistakenly attributed to the “aging process”. Due to this, many of us have our tales of the long road – through many medical missteps — to finally receiving the proper diagnosis.
I can’t pinpoint when my symptoms began because they all started around the same time. These symptoms were difficulty walking, mild dementia, and impairment in my bladder control. However, sadly, my doctors failed to “connect the dots.” It was only when my worsening symptoms forced me to abruptly retire — and move to a new city — that my new Primary Care Physician did, finally, connect the dots. In our first meeting, he said “You have the three symptoms of Normal Pressure Hydrocephalus.” To which I replied, “What’s that?”
But I am one of the “fortunate” ones. It is estimated that more than 800,000 Americans have NPH, but less than 20% receive an appropriate diagnosis. What many people do not know is that NPH is one of the few treatable forms of dementia. I believe this is “the elephant in the room” that nobody wants to discuss. We need to each do our part to raise awareness about NPH!
Have you ever heard of, “wet, wacky, and wobbly”?
I smiled when I first heard about “the three w’s,” an old shorthand mnemonic that some people use when talking about three of the symptoms of NPH. Since space is limited here, I will assume those of you reading this already know what the three w’s mean.
- wet represents the symptom of incontinence (impaired bladder control)
- wacky represents cognitive impairment (mild dementia)
- wobbly represents gait disturbance (difficulty walking)
It’s important to know these symptoms may not all occur simultaneously and can emerge at different stages with varying levels of severity. Likewise, your treatment method may improve your symptoms differently than other NPH patients.
It’s estimated that more than 80% of those properly diagnosed with NPH and screened for shunt responsiveness will experience rapid improvement in their condition, although it may take weeks or months to see the full benefits of the procedure.
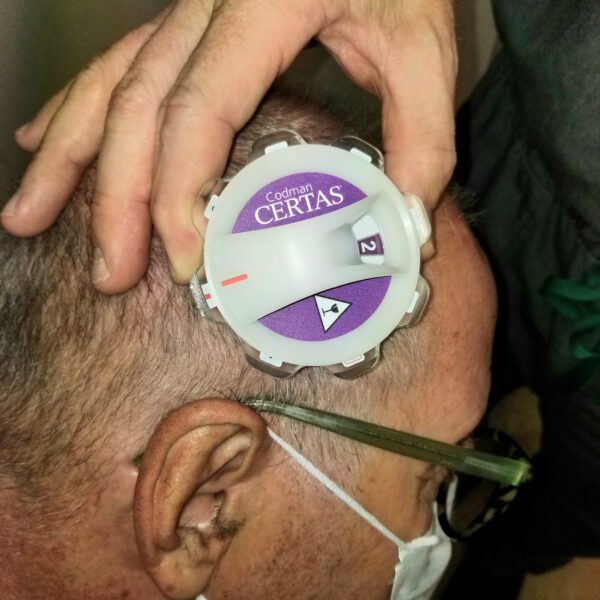
I went into my first shunt surgery very naïve about my shunt, confident that the surgery would “cure” my NPH. It’s important to note that a shunt is not a cure.
So, what now?
Following my last shunt revision, a physician’s assistant gave me advice that has provided the foundation for dealing with NPH. She said, “manage your expectations.” At that moment, I was still on pain meds and a bit disoriented. Her advice sounded pessimistic, but over time, it has proven to be true.
Today, I am grateful for any improvements provided by the treatment I have received, with the full knowledge that my recovery may be imperfect. And, yes, my doctors and therapists gently remind me that — NPH or not – “no 74-year-old brain functions the way it used to, Frank.” The most significant improvement from my ventriculoperitoneal (VP) shunt was in gait and balance.
My cognitive abilities are better sometimes and worse at other times. I try to tackle the important cognitive tasks during the welcome — but unpredictable — “moments of clarity” in my day. I try to give myself grace when my brain can’t manage the challenging times. The most troublesome symptom of my cognitive impairment is apathy, which is also very common among many of my peers. As for incontinence, I recently had a sad anniversary – it has been seven years since I have been able to wear underwear. I have accepted that I will likely wear adult pull-ups for the rest of my life. It’s not the worst outcome, I tell myself. I’m still here.
I am grateful for the many blessings in my life. But I won’t sugar coat it. There are dark days, when I retreat to my bed and sleep for 36 hours, feeling defeated and depressed, fearful that I won’t be able to continue to live independently. But there are also moments when I feel cautiously optimistic that, with the support of my family, friends, medical team, and the thousands of my fellow “hydro warriors” that I will be OK in this “new normal”.
Please click here to read Living With NPH Part 2: Tips for Living With NPH
