Posts Tagged ‘premature’
New Study Seeks to Improve Outcomes After a Brain Bleed
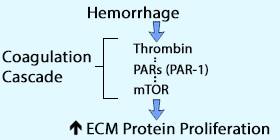
Germinal matrix hemorrhage (GMH) is a brain bleed that occurs in approximately 3.5 per 1000 live births and remains a leading cause of mortality and lifelong morbidity in premature infants.
Read MoreLooking Back…Moving Forward: From the NICU to Medical School
Jennifer Bechard sits down with Jamie Wright, our Support Group Leader in Houston, TX, as we continue our history series commemorating our 30th anniversary. Jamie was born six weeks prematurely, diagnosed with post-hemorrhagic hydrocephalus, and was shunted at 20 months old. She is now in her second year of medical school at the University of Texas Medical School at Houston, where she is in a combined MD/PhD program.
Read More