Posts Tagged ‘ETV’
Research 101: Generalizability
The concept of Generalizability in research studies is especially important for individuals living with hydrocephalus because there are so many different causes.
Read MoreChanging Treatments: Converting from a Shunt to an ETV for the Treatment of Hydrocephalus
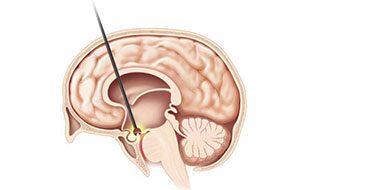
A recent study published in Neurosurgery looked at the success rate of converting from a shunt to an endoscopic third ventriculostomy (ETV) in pediatric and young adult patients. The study, with lead author Dr. David S. Hersh, retrospectively reviewed patient data from three children’s hospitals in the United States.
Read MoreDoes the size of an Endoscopic Third Ventriculostomy (ETV) hole increase over time?
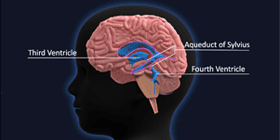
This study is the first to evaluate the size of the ETV hole using MR imaging over a period of time. This research is important because it shows us how useful MR imaging can be to neurosurgeons who want to evaluate an ETV.
Read MoreShunt versus ETV: Five year outcomes from the International Infant Hydrocephalus Study (IIHS)
The IIHS gathered data from more than 20 hospitals around the world, compared the effectiveness of shunts versus endoscopic third ventriculostomies (ETVs). This study started in 2005 and these are the five year outcomes.
Read MoreIs an ETV an Option After Shunt Failure?
Is an ETV an option after shunt failure? A recent review of 15 studies reported on the effectiveness of endoscopic third ventriculostomy (ETV) after shunt failure in children. Dr. Jenna Koschnitzky, National Director of Research Programs, summarizes the findings.
Read MorePreliminary results from the International Infant Hydrocephalus Study
There are two common treatment options available for infants that suffer from Aqueductal stenosis: implantation of a shunt or an endoscopic third ventriculostomy
Read MoreNew Tool Detects Pressure Non-invasively
Non-invasive tool may be instrumental in evaluating elevated ICP – a symptom of hydrocephalus and shunt malfunction.
Read MoreOver 500 Adult Hydrocephalus Patients Enrolled in Registry
HA is proud to fund the AHCRN as they move research from bench to bedside to find new treatments, preventions and cures for adults living with hydrocephalus and NPH.
Read MoreAnnouncing Our 2016 Hydrocephalus Association Scholarship Recipients!
The Hydrocephalus Association (HA) is pleased and honored to announce our 2016 Hydrocephalus Association Scholarship Recipients.
Read MoreHydrocephalus Receives National Attention
TLC aired a feature piece on hydrocephalus that featured three families – Roona in India, Lyndos in Uganda, and Parker in Oklahoma.
Read MoreWhy I WALK – For a Better Tomorrow
The WALK has become so important to me because I know how it feels to be alone and confused after being diagnosed with hydrocephalus.
Read MoreMixed Emotions: Heartbreak
Jamie Wright, Houston Community Network leader, went to Haiti with a pediatric neurosurgery team from Children’s Memorial Hermann Hospital. This is her experience.
Read MoreRealizing I Had Hydrocephalus
Dan Kricke talks about the first time he realized he had hydrocephalus when he was 5 and the various emotions he had along the way to adulthood.
Read MoreTelling My Story
Meet Dan, a new guest blogger lending his voice to our adult hydrocephalus community. We are excited for Dan to share different aspects of his journey each month.
Read MoreMaking the Hydrocephalus Association a Part of My Legacy
At the age of 25, Haylea is thinking about how she will make a lasting impact in the hydrocephalus community through her volunteerism and estate planning.
Read MoreEndoscopic Third Ventriculostomy (ETV) in Children: Prospective, Multicenter Results from the Hydrocephalus Clinical Research Network (HCRN)
What determines the success of an ETV for treating hydrocephalus? Dr. Kulkarni shares their initial findings gathered from across HCRN centers.
Read MoreHydro Queen
Karly Rodriguez wrote this powerful and honest poem one month prior to her ETV procedure, after being diagnosed with hydrocephalus in 2012.
Read MoreLooking Back…Moving Forward: The Need to Value Shunt Management
As the Hydrocephalus Association continues our 30th anniversary interview series, Ann Marie Flannery, M.D., shares her thoughts on young adults transitioning to adult neurological care and issues a call to action for society to value the management of shunts and the individuals living with them.
Read MoreLooking Back…Moving Forward: Adding a Touch of Pixie Dust
Tina Daniels, Hydrocephalus Association Support Group leader in Owasso, OK, shares her experiences living with hydrocephalus and her decision to lead a support group.
Read More