Let’s Navigate this together
Trusted resources to help you on your journey.
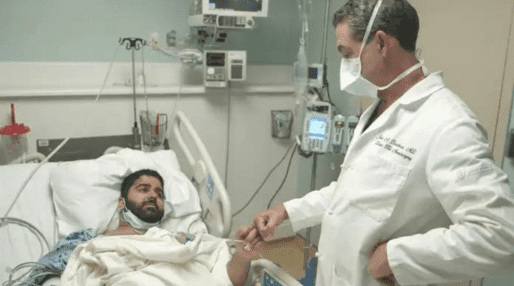
Recently Diagnosed?
Have you or a loved one recently been diagnosed with hydrocephalus?
Tools for Daily Life
Learn how to manage the day to day symptoms and challenges you might encounter on your journey with hydrocephalus.
Get Support
We're here to help! Find the support you need and talk to people who know what you're going through.
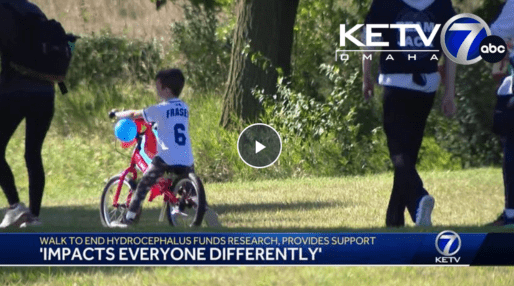
Make An Impact
We come together in so many ways — all of us driven by a passion to find a cure and improve the lives of those impacted by hydrocephalus. Whether you participate in a WALK to End Hydrocephalus or join our advocacy efforts, you’re making a difference!
Connect With Us
When you're ready, let's take the next step together. Stay informed with our monthly newsletter! We'll share inspiring stories, and information about our programs, events, and research.